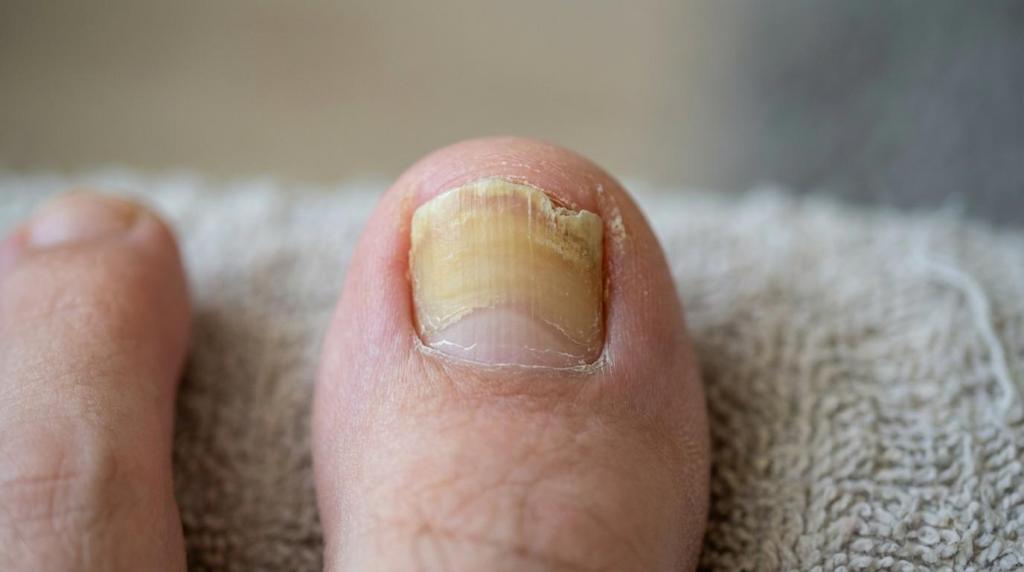
Toenail fungus can feel stubborn in a way that’s hard to explain until you’ve lived with it. You trim the nail, try multiple over-the-counter liquids, maybe even a prescription topical, and the discoloration and thickening keep coming back. That frustration is valid, and it’s also a clue: many established toenail infections live deep under the nail plate, where many topicals struggle to reach.
Oral terbinafine has long been considered a first-line prescription option for dermatophyte toenail fungus, and “pulse dosing” is one evidence-supported way clinicians may prescribe it for the right patient.
Meta description: Pulse-dose terbinafine is an intermittent oral regimen for toenail fungus that can offer similar cure rates to daily dosing with less total medication. Learn typical schedules, safety monitoring, timelines, and how STRIDE’s doctor-led online care supports results.
Pulse dosing is an intermittent schedule: you take a higher dose for a short, defined window, then stop for a longer “off” period before the next pulse. This differs from the standard continuous regimen of terbinafine 250 mg once daily for about 12 weeks for toenail fungus.
Why would anyone stop an antifungal on purpose? Because terbinafine concentrates in keratin and can remain in the nail and surrounding tissue at antifungal levels long after the last tablet. That persistence is one reason intermittent dosing has been studied in onychomycosis (nail fungus), and why many clinicians consider it a practical option when it fits the clinical picture.
Pulse dosing for toenails is commonly discussed as 500 mg/day for 7 days repeated every 4 weeks for 3 to 4 pulses in clinical studies. Some protocols also use longer gaps between pulses. At STRIDE (by Distinct Dermatology), clinicians may prescribe pulse-dose terbinafine in a schedule designed to balance results and safety, and it can differ from the “monthly pulse” you may see online.
Most OTC products are limited by penetration. Toenails are dense keratin. When fungus is established under or within the nail plate, topical medication often cannot reach the organisms in high enough concentrations for long enough.
Oral terbinafine works systemically, reaching the nail unit through blood flow. It’s most effective against dermatophytes (commonly Trichophyton species), which are a leading cause of classic toenail fungus. That detail matters because not every thick, yellow nail is dermatophyte onychomycosis.
A key part of safe prescribing is making sure you are treating the right condition. Many clinicians confirm the diagnosis with testing (microscopy, culture, or molecular testing) when the presentation is unclear, severe, or has failed multiple rounds of treatment.
Your exact dosing plan should come from a clinician who has reviewed your medical history, current medications, and nail severity. Still, it helps to see the patterns.
Here is a plain-language comparison of commonly used approaches, including the type of pulse schedule often used in STRIDE’s protocol.
[markdown] | Approach | What patients take | Typical “active treatment” window | Why it’s used | | --- | --- | ---: | --- | | Continuous terbinafine (standard) | 250 mg by mouth once daily | ~12 weeks | Simple routine; strong evidence base | | Monthly pulse terbinafine (studied regimen) | 500 mg/day by mouth for 7 days, then ~3 weeks off, repeated 3 to 4 times | ~3 to 4 months (intermittent) | Similar cure rates in studies with fewer total tablets | | Longer-interval pulse terbinafine (one investigated option) | 500 mg/day by mouth for 7 days with longer off periods between pulses | Can extend over many months | Designed around terbinafine persistence in nails | | Dual therapy (oral + topical) used by STRIDE | Pulse-dose oral terbinafine paired with a compounded topical designed to improve nail penetration | Oral pulses plus ongoing topical use | Targets fungus from inside and outside; supports higher cure rates in teledermatology protocols | [/markdown]If you are comparing “how long treatment lasts,” it’s also important to separate how long you take medication from how long it takes to see a clear nail. Even after the fungus is eliminated, damaged nail has to grow out.
For dermatophyte toenail fungus, multiple studies and a meta-analysis have found that pulse-dose terbinafine can deliver comparable mycological cure rates to continuous dosing, with similar rates of reported adverse effects. Some individual studies show small differences one way or the other, but overall the data support pulse dosing as a reasonable option in appropriate patients.
Two points patients often find reassuring:
That said, no regimen is perfect for everyone. Severe nail thickening, extensive nail involvement, mixed infections, and reinfection risk from shoes or shared surfaces can all affect outcomes regardless of schedule.
Most people tolerate terbinafine well, but it is still a prescription systemic medication with real risks. The most common side effects include gastrointestinal upset, headache, rash or itching, and taste disturbance. Liver enzyme elevations occur in a small percentage of patients, and clinically significant liver injury is rare but serious.
Before starting terbinafine, clinicians typically review:
Because safety does not “turn on” only with long courses, pulse dosing does not remove the need for careful screening. It reduces total exposure, yet rare reactions have been reported even after short courses, so patients still need clear guidance.
Many clinicians recommend baseline liver function tests (LFTs) before oral terbinafine. Follow-up testing depends on your plan, duration, risk factors, and whether symptoms appear.
If you are prescribed terbinafine, ask what monitoring your clinician wants for your specific situation and how to reach the care team quickly if something feels off.
Here are symptoms that generally deserve prompt medical contact, especially if they are new and unexplained:
Do not try to “push through” severe symptoms to finish a pulse. A clinician would rather hear from you early, reassess, and keep you safe.
A practical timeline many clinicians share looks like this:
It is also common for one or two nails to lag behind the others. Severity at baseline matters: very thick nails or nails lifted off the nail bed often take longer and may need added measures (thinning, targeted topical penetration strategies, shoe hygiene).
STRIDE’s core strategy is a dual-therapy plan, often called STRIDE DUO: clinician-supervised oral antifungal pulse therapy plus a compounded topical designed for nail penetration (STRIDE ClearNail Renewal™ includes keratolytics like urea and lactic acid combined with an antifungal).
The goal is simple: treat fungus from the inside while also addressing the nail environment from the outside, where reinfection and residual organisms can persist.
Patients often choose STRIDE because it combines:
STRIDE reports high cure rates with its science-driven protocols, including “up to 89%” in program materials. As with any medical outcome, your results depend on diagnosis, severity, adherence, and risk factors, so a clinician should help you set a realistic target and timeline.
Pulse regimens are straightforward, but the “on week” matters. During each pulse, take the medication exactly as prescribed. Some clinicians direct 500 mg/day as two 250 mg tablets, sometimes taken together, sometimes split into morning and evening doses.
A few practical habits improve consistency and tolerability:
If you miss a dose, the best next step depends on where you are in the pulse week and how your clinician structured your plan. Many prescribing instructions advise taking the missed dose when remembered unless it’s close to the next dose, but you should follow your clinician’s guidance and the prescription label. If you miss multiple doses in a pulse, it’s worth checking in rather than guessing.
Toenail fungus care works best when treatment and prevention run together. Ongoing tracking is not busywork; it helps your clinician spot slow response, mixed disease, or signs that the nail is growing out normally.
Here are simple actions that often make a measurable difference over months:
If you have athlete’s foot (tinea pedis) at the same time, treating the skin matters because it can reseed the nails.
Some patients cannot take terbinafine safely, and a good program should have alternatives. Fluconazole is a common option when terbinafine is not appropriate, typically taken weekly for a longer period.
Also, some nail problems look like fungus but are not, including psoriasis, trauma-related dystrophy, and chronic nail irritation. If you have tried multiple treatments without any change, it’s a signal to get a clinician’s review and consider diagnostic testing before repeating another course.
Many adults delay treatment because scheduling in-person visits and pharmacy pickups is one more task on an already full calendar. STRIDE’s model is designed around convenience without skipping clinical oversight: an online evaluation, prescription delivery to your door in discreet packaging, and support while your nail grows out.
If you’re considering pulse-dose terbinafine for toenail fungus, the most helpful next step is a clinician review of your nail photos, medical history, and medication list. Questions are welcome, and you should feel comfortable asking about dosing options, lab monitoring, expected timelines, and what “success” should look like for your specific nails.