A toenail that suddenly looks “off” can be surprisingly hard to interpret. A bruise from a long run, a tight shoe, or a dropped object can discolor and distort a nail in ways that resemble infection. At the same time, true toenail fungus can start subtly, then progress until the nail thickens, crumbles, and lifts.
The stakes are practical: treating the wrong problem wastes months, and many nail conditions can mimic fungus. STRIDE’s clinical guides emphasize that you should not guess, since a large share of nails people assume are fungal turn out to be something else after medical review.
Both trauma and fungal infection can change nail color and texture, and both can make a nail look dull, rough, or partially detached. Even clinicians often rely on pattern recognition plus confirmation testing when the story is not clear.
One simple difference is timing. Injury changes tend to be linked to a specific event and show up quickly. Fungal infection usually develops slowly and tends to worsen over months, not overnight.
Toenail fungus (onychomycosis) most often causes gradual discoloration, thickening, brittleness, and crumbly debris. STRIDE’s educational content highlights several classic features:
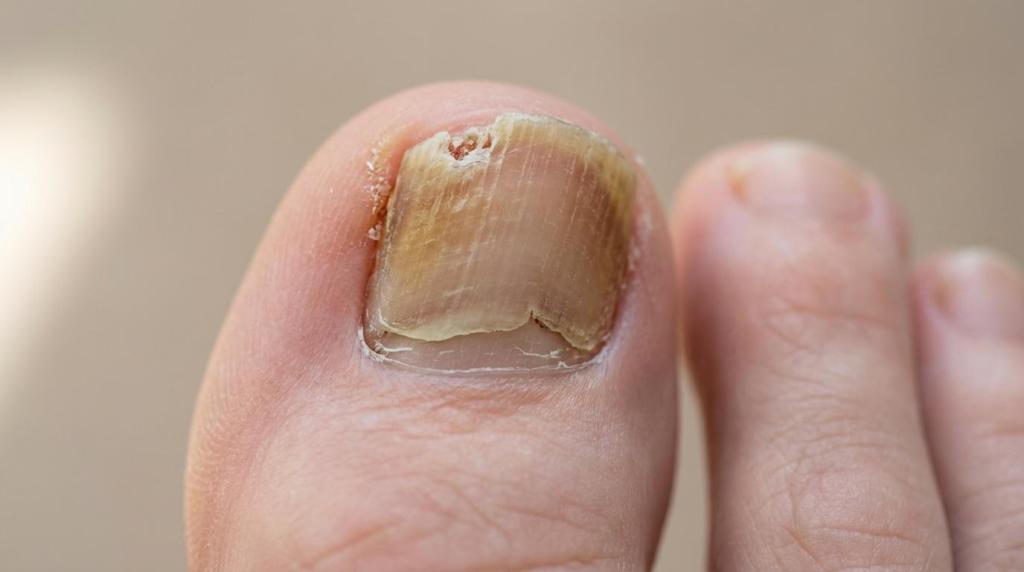
Color changes often skew yellow, brown, white, or greenish, and the nail may become thicker and harder to trim. As infection progresses, the nail plate can become ragged and distorted, and it may begin lifting from the nail bed (onycholysis). Some people notice an odor, which can happen when debris builds up under the nail.
Fungus also tends to start at the tip or edges of the nail and slowly spreads toward the base.
Trauma is usually more “event-based.” Think stubbing a toe, dropping a weight, repetitive pressure from tight footwear, or sudden mileage increases in running. A bruised nail often shows dark red, purple, brown, or black discoloration under the nail from trapped blood (a subungual hematoma). Pain or tenderness is common early on, especially in the first day or two.
Some injuries cause the nail to loosen, split, or eventually fall off, then regrow over many months. In chronic microtrauma, the nail can look thick or ridged as it grows out, which is one reason it can be mistaken for fungus.
A key clue is speed: an injury usually looks worse quickly, while fungus tends to creep.
These patterns are not perfect, but they are useful when you are deciding whether to try home care, monitor growth, or seek a clinician’s evaluation.
[markdown] | Feature | More consistent with toenail fungus | More consistent with bruised/injured nail | | --- | --- | --- | | Typical color | Yellow, brown, white, sometimes greenish | Dark red, purple, brown, black under the nail | | Onset | Gradual, over weeks to months | Sudden after impact or within days of pressure/friction | | Progression | Slowly worsens, spreads from tip/edges toward base | Stays localized, then “grows out” with the nail | | Thickness | Nail commonly thickens and becomes hard to trim | Can look thick during regrowth, but not always | | Texture | Brittle, crumbly, ragged edges; debris under nail | Surface may be smooth; nail may crack or split after trauma | | Under-nail debris | Common | Uncommon (unless fungus is also present) | | Pain | Often minimal | Often tender or painful early; severe pain suggests injury or another problem | | Pattern across nails | Can involve multiple nails, often both feet | Often one nail, tied to a specific toe or activity | [/markdown]After you have looked at the nail in good light, it helps to do a structured check rather than focusing on one detail.
Here are quick observations to write down before you seek care or start treatment:
Those notes may sound basic, but they map closely to how clinicians triage nail problems.
If you are deciding between “watch it grow out” and “get evaluated,” use time as data.
Start by answering three questions: When did it begin, how fast did it change, and is it moving as the nail grows?
This is not a replacement for diagnosis, but it often prevents people from treating for fungus when the nail is simply growing out an injury.
Some nail changes should not be watched at home, even if you suspect trauma or fungus. STRIDE’s guidance flags symptoms that are less typical for straightforward fungal infection and need clinician review.
If any of the following are true, prioritize professional evaluation:
One sentence that is worth repeating: a nail that looks abnormal is not always fungal.
Over-the-counter antifungal products are widely marketed, but fungal toenails are hard to clear without the right plan and enough time. If the nail problem is actually trauma, psoriasis, eczema, or another condition, months of antifungals can become expensive delay.
Mislabeling also cuts the other way. If a true fungal infection is ignored for a long time, it commonly progresses, thickens the nail, and can lead to discomfort in shoes. STRIDE’s educational resources emphasize early evaluation because fungal nails often worsen slowly and can deform the nail plate as time passes.
A careful history and close visual review often narrow the possibilities, especially with good photos and a timeline. Still, nails can be deceptive.
When confirmation is needed, clinicians may order lab testing on nail clippings or subungual debris. Common approaches in dermatology include microscopy (often with KOH prep), fungal culture, and pathology staining (often PAS) to look for fungal elements within the nail. The goal is straightforward: confirm fungus before committing to months of treatment, especially when oral medication is being considered.
STRIDE’s doctor-led approach centers on photo and history-based evaluation first, with the option to order lab work when appropriate.
Toenail fungus is rarely a quick fix. Nails grow slowly, and clearance depends on both killing the organism and allowing healthy nail to grow in.
Many people start with topical-only products and get limited results, especially when the nail is thick or the infection is longstanding. Evidence-based care often uses oral therapy, topical therapy, or a combination, depending on severity and medical history.
A common clinical strategy is dual therapy: an oral antifungal to treat infection from within plus a topical to improve local control and penetration. STRIDE’s doctor-led approach reflects this, pairing clinician-supervised oral options (terbinafine or fluconazole when appropriate) with advanced compounded topicals designed to penetrate thickened nail.
In eligible patients, pulse dosing is sometimes used to reduce total exposure while maintaining effectiveness. One example used in structured protocols is pulse-dose terbinafine taken in short cycles with breaks, under clinician supervision, with attention to safety and medication interactions.
Most minor nail trauma improves with time and protection. The goal is to reduce repeated pressure and allow the new nail to grow without continued damage.
A few practical steps often help:
If there is a very painful blood collection under the nail soon after injury, urgent care can sometimes relieve pressure. Do not attempt drilling or draining at home.
Photos are often good enough to triage fungal patterns vs injury patterns, but only if they are sharp and well-lit. Take photos after gently washing and drying the foot, then use bright natural light.
A simple photo set that helps clinicians is:
If you are not sure whether your nail is fungus or trauma, this is often the fastest way to move from guessing to a plan.
Many adults seek help after years of cycling through polishes, home remedies, and even prior prescriptions without lasting clearance. That pattern is common when the original diagnosis was never confirmed, when treatment was too mild for the severity, or when adherence is hard to maintain.
STRIDE (by Distinct Dermatology) offers nationwide teledermatology for toenail fungus with board-certified clinician oversight, prescription options including oral therapy when appropriate, custom-compounded topical solutions, discreet shipping, and ongoing support with progress tracking. For people who want to avoid office visits and still get medically supervised care, that model is designed to make diagnosis and treatment more straightforward.
If your nail changed overnight after a clear injury, you may mainly need time and protection. If the nail has been slowly thickening, crumbling, lifting, or spreading from the edges for months, it is worth getting evaluated so you can stop guessing and treat what is actually there.