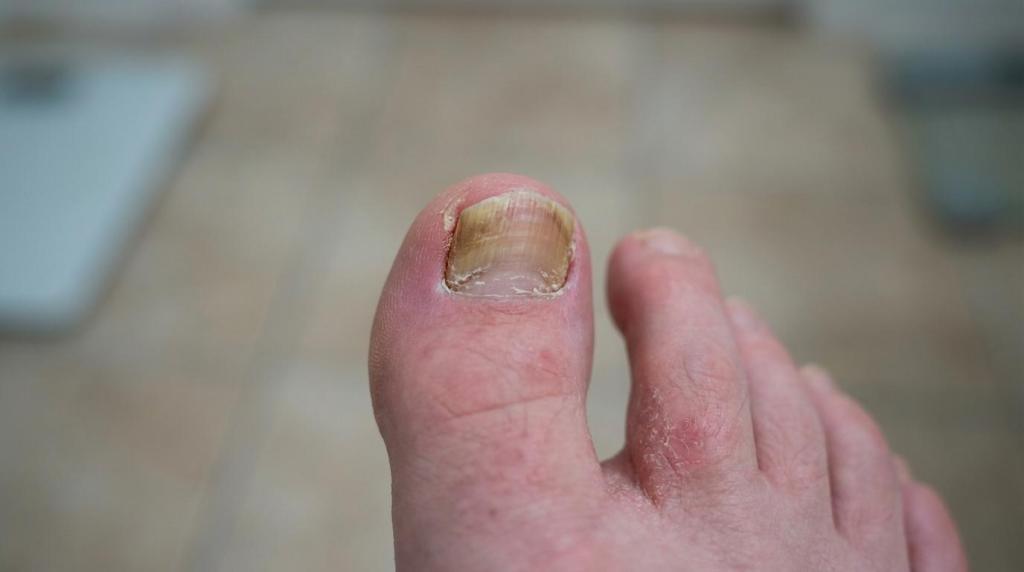
Toenail fungus can feel like it comes out of nowhere. A nail that used to look normal starts turning yellow, thickening, or crumbling at the edge. You try a drugstore polish or a home remedy, it improves a little, then months later it looks the same again.
That pattern is common because a fungal nail infection is not just “surface discoloration.” It is a slow-moving infection inside a structure that grows slowly, gets little immune surveillance, and spends most of the day inside warm, closed shoes.
Clinicians usually call toenail fungus onychomycosis. In most cases, fungi colonize the skin first (often athlete’s foot), then move under the nail’s free edge or along the sides and settle into the space between the nail plate and the nail bed.
Once the fungus is established, it feeds on keratin and triggers thickening, debris, and partial lifting of the nail. That lifting creates more space for moisture and organisms, which makes the infection harder to clear.
Toenails also grow slowly, often only 1 to 2 mm per month. So even when treatment works, you typically have to wait for healthy nail to grow out to see a clear result.
Most toenail fungus is caused by a specific group of fungi that prefer keratin. These are not rare “tropical” organisms. They are common in day-to-day environments, especially where feet are warm and damp.
Here’s the practical breakdown clinicians use:
[markdown] | Fungal type | Common examples | Approximate share of toenail infections | Typical clues and context | | --- | --- | ---: | --- | | Dermatophytes | Trichophyton rubrum, T. mentagrophytes, Epidermophyton floccosum | ~90% | Often linked with athlete’s foot, occlusive shoes, communal wet floors | | Yeasts | Candida species | ~2% | More common in fingernails; can occur with immune suppression or chronic moisture exposure | | Nondermatophyte molds | Fusarium, Aspergillus, Scopulariopsis, others | ~5 to 10% | More likely after nail trauma, in older adults, or with circulation problems | [/markdown]Why does this matter? Because drug choice and expectations change depending on the organism, the nail’s thickness, and how much of the nail unit is involved. Dermatophytes tend to respond best to terbinafine, while some molds and yeasts may require different strategies.
Fungus typically needs two things: exposure and an entry point.
Exposure happens when fungal spores land on the skin, often from floors, towels, shoes, or shared grooming tools. Entry points happen when the skin barrier is disrupted, the nail separates slightly from the bed, or the side nail folds get irritated.
Common “entry ramps” include:
Athlete’s foot is a frequent starting point. Skin fungus can quietly persist between toes, then keep re-seeding the nail area over time.
Fungi thrive in moisture. Feet spend hours in shoes where sweat cannot evaporate well, creating a stable, humid microclimate. Add friction and pressure, and the nail becomes more vulnerable to tiny separations that let organisms in.
Communal wet areas raise exposure risk because fungal spores can be present on surfaces where many people walk barefoot. Gyms, locker rooms, pool decks, and shared showers are classic examples. Occupational data also supports this: swimming-pool employees have shown much higher rates of onychomycosis and combined nail infection plus athlete’s foot than controls in published research.
Home is another overlooked source. Fungal spores can persist in shoes and textiles, and research suggests T. rubrum can survive typical lower-temperature laundry cycles, with higher heat being more reliable for killing organisms. If socks, footwear, or bathroom floors stay contaminated, a “cleared” nail can be exposed again and again.
A returning infection can be a true relapse (the original infection was never fully eradicated) or a reinfection (a new exposure lands on a susceptible nail). Both are common, and they often overlap.
Several biology and lifestyle factors make recurrence more likely.
After a nail infection has been present for a while, it can behave less like a simple surface infection and more like a protected colony living inside keratin.
Recurrence is not a personal failure. It is often a predictable outcome when the organism is protected by nail structure, the environment keeps exposing the foot, or the treatment plan does not match the severity of disease.
Some people are simply more vulnerable, even with good hygiene. Risk increases when nail growth slows, circulation is reduced, immune function is impaired, or the nail is repeatedly traumatized.
This comes up often in clinical care:
If you have diabetes or circulation problems, nail fungus is more than cosmetic. Thickened nails can contribute to pressure points, skin breakdown, and secondary bacterial infection.
Yellow or thick nails are not always fungal. Trauma, psoriasis, eczema, and certain nail growth disorders can look similar. Even clinicians often confirm with a lab test before committing someone to months of treatment.
Testing can include microscopy (KOH), fungal culture, or histology (PAS stain). Confirmation matters because it helps avoid months of effort spent treating the wrong condition.
Drugstore products are popular because they are easy to buy, but most do not penetrate the nail well enough to clear established toenail infections. Even prescription topicals have modest complete cure rates in studies, especially when the nail is thick or more than a small portion is involved.
Oral antifungals generally have higher mycologic cure rates. Oral terbinafine is often considered first-line for dermatophyte infections, with fluconazole used in some situations when terbinafine is not a good fit. These medications still require medical screening for interactions and safety, and some patients need lab monitoring based on health history.
Many clinicians also use combination approaches, because nails are a tough target. Pairing systemic therapy with a topical that improves penetration, plus thinning or trimming thick nail, may raise the odds of success in harder cases.
STRIDE (by Distinct Dermatology) is one example of a doctor-led teledermatology option focused on toenail fungus, including dual-therapy protocols that combine oral antifungals with a compounded topical designed to penetrate better. It is fully online, which can help patients who want privacy and consistent follow-up, and it can be especially helpful for people who have already tried over-the-counter products without results. The key is clinician oversight so the plan fits your medical history, organism likelihood, and nail severity.
Treatment works best when you also reduce re-exposure. That does not mean sterilizing your entire life. It means cutting down the most common reservoirs.
Start with the basics: keep feet dry, change socks daily (more often with heavy sweating), and rotate shoes so they fully dry between uses. Treat athlete’s foot at the same time as nail fungus, even if it seems minor.
A simple prevention routine often includes:
If pedicures are part of your routine, bring your own tools or confirm sterilization practices. Small skin nicks around the nail fold can become entry points.
If the nail is painful, swollen, draining, or suddenly dark, get evaluated promptly. Also seek care sooner if you have diabetes, reduced sensation in your feet, poor circulation, or immune suppression.
Toenail fungus is common, treatable, and worth addressing early. The longer it sits, the more nail it tends to involve, and the harder it becomes to clear and keep clear.